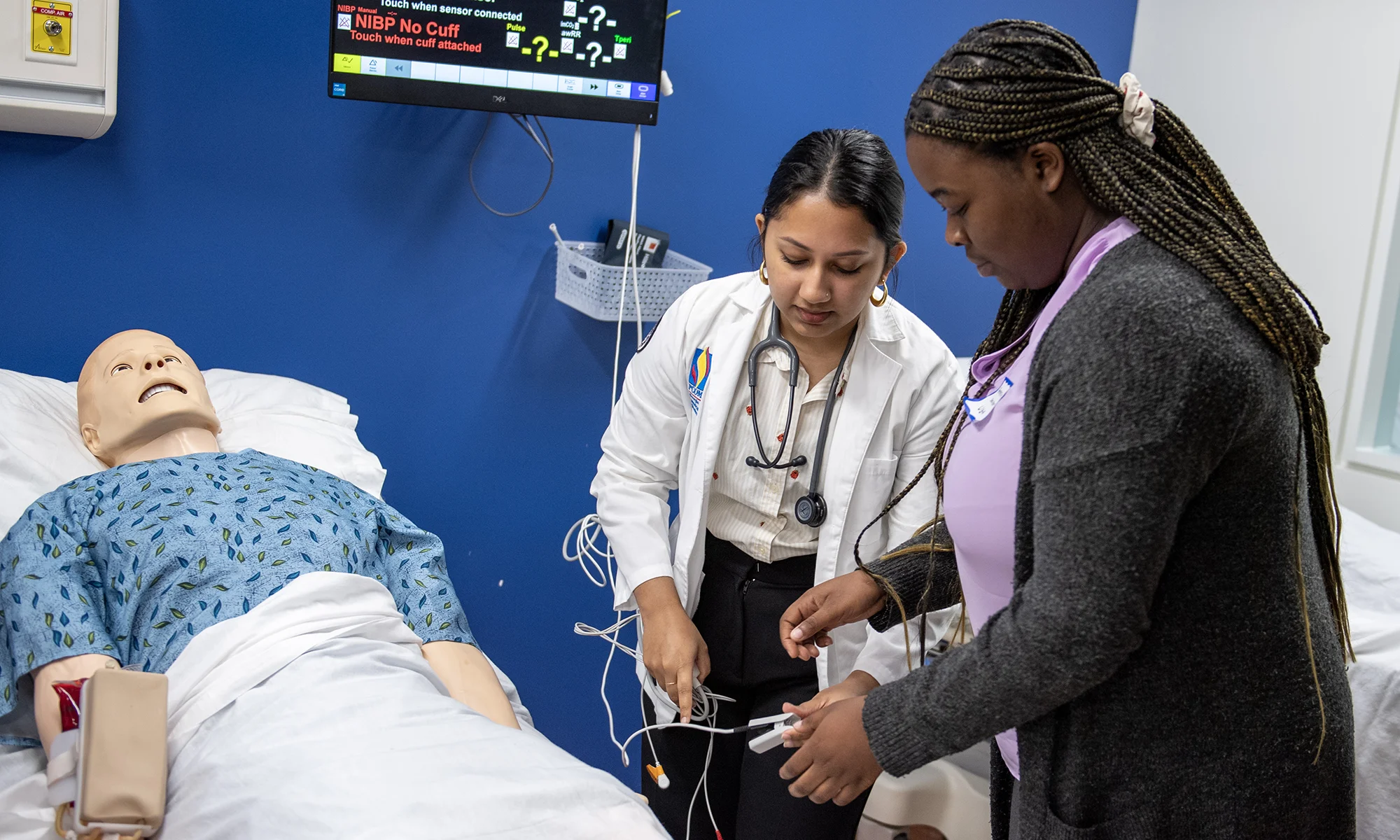
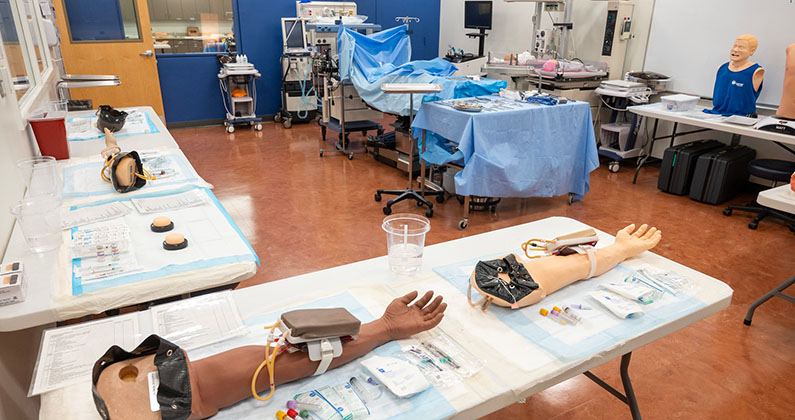
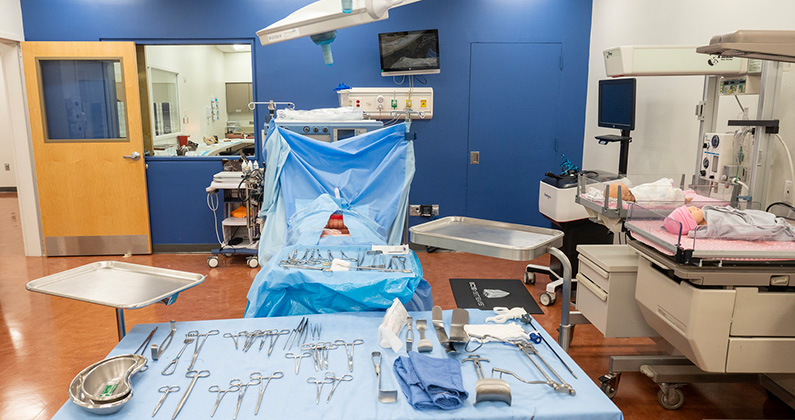
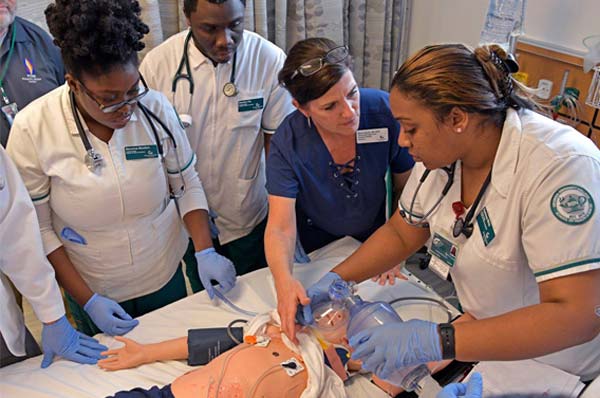
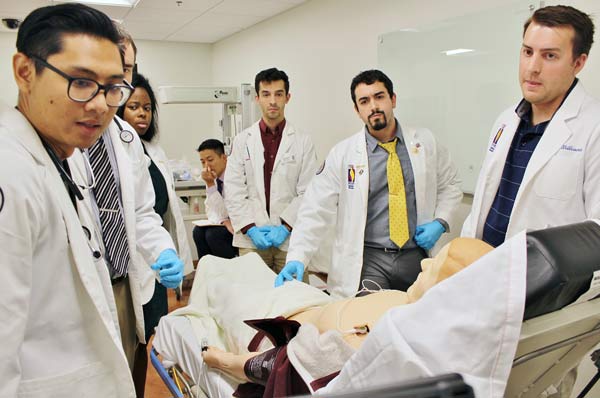
The mobile simulation lab is a teaching tool for trauma and pre-hospital care. The
lab resembles an ambulance and houses modern emergency equipment including vital monitors,
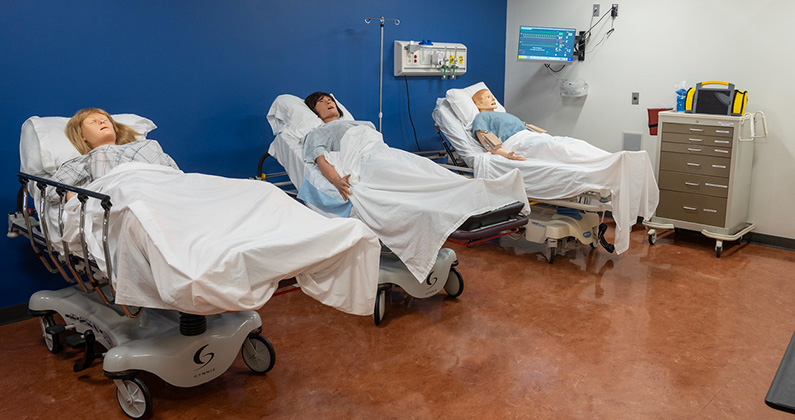
stretchers, splints, suctioning equipment, intubation equipment, simulated medications
and much more. In addition, equipment and patient mannequins found in the Simulation
Center can be moved into the mobile lab.
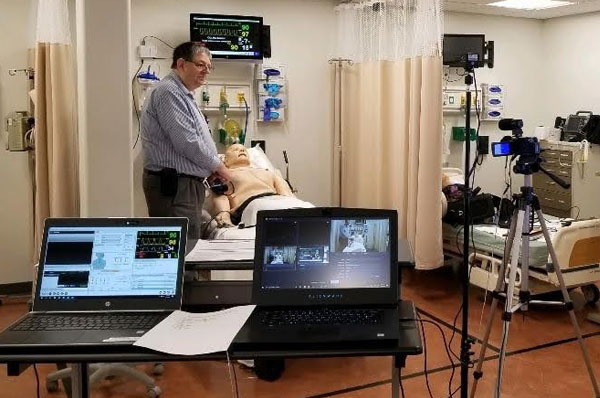
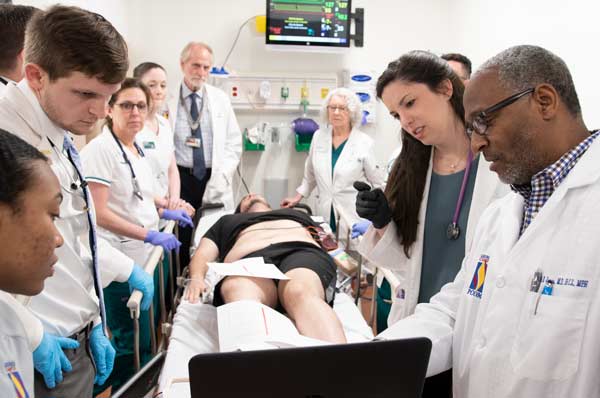
Emergency simulations are conducted inside and around the vehicle. Doctoral and medical
simulation students can practice a variety of scenarios including cardiac arrest,
childbirth, bone fractures, burns, gunshot wounds, allergic reactions, overdoses and
more.
The lab is used to teach both PCOM Georgia and PCOM South Georgia learners when it
makes trips between the two locations. It is also used during community education
events such as the Gwinnett Science Fair or training events held in conjunction with neighboring institutions and EMS stations.